Sciatica
Everything You Need To Know About Sciatica
Physiotherapy can be very effective for relieving sciatica pain. Your physiotherapist can also design an exercise program to strengthen and improve the mobility of your back, leaving you less vulnerable to bouts of sciatica. One of the most common causes of sciatica is a disc herniation in the lumbar spine. When the herniated disc impinges or compresses a nerve root, sciatica can occur. 90% of patients with a lumbar disc herniation improve without a medical intervention like surgery within 3-6 months.
Signs and Symptoms of Sciatica
- Pain that starts in your lower back or your buttock and travels down the back of the leg.
- Pain can be an ache or a sharp burning sensation.
- Pain can worsen with coughing, or sneezing this can indicate lumbar disc pathology or spinal hypermobility.
- Some patients feel numbness or tingling or ankle muscle weakness on the affected side.
- Severe symptoms include trouble walking due to pain.
Causes of Sciatica
- Sciatica happens when the sciatic nerve becomes compressed or inflamed.
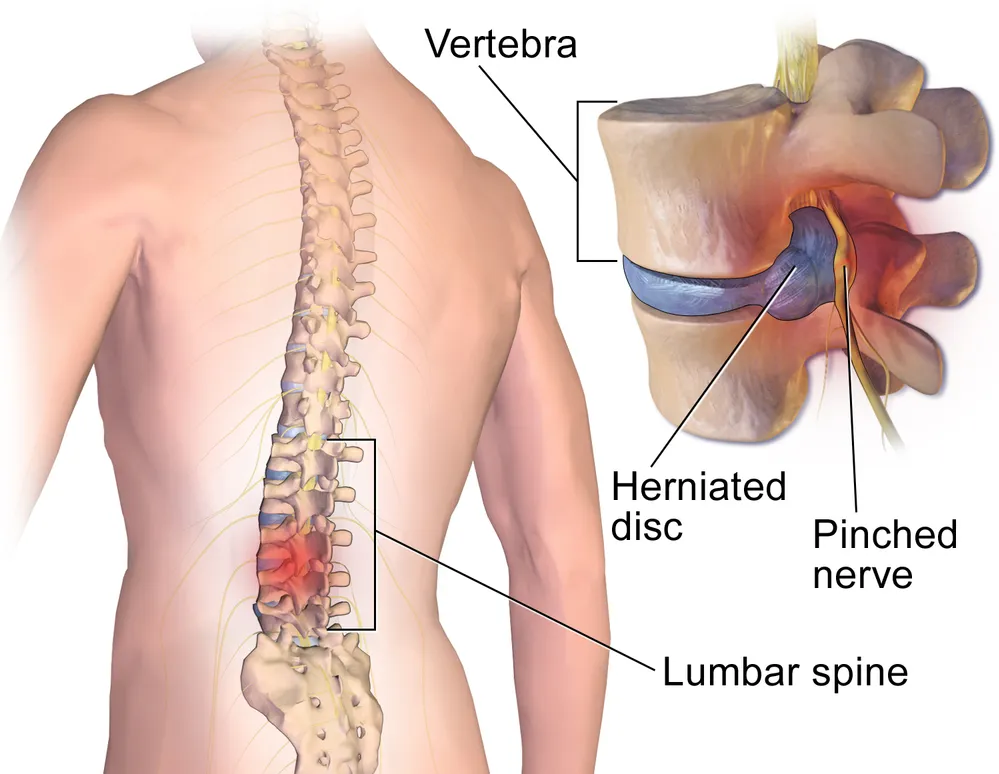
- There are discs between the bones of your spine (vertebrae) that act as shock absorbers. Sometimes they can bulge or herniate creating a local inflammatory response and pressure on the nerve. This is the most common cause of sciatica.
- Bony changes called “bone spurs” can press on nearby nerves in a spine that suffers from arthritis.
There is a muscle that lies deep within your buttocks called the piriformis muscle. It has been suggested that this muscle can become tight or spasm which can put pressure on the sciatic nerve, though this is rare. Sometimes other medical conditions (like tumours) can injure nerves near the spine.
Sciatica Risk Factors
- With advancing age, our spines go through a degenerative process that includes disc bulges, herniations and the development of arthritis. These conditions increase your risk of experiencing sciatica.
- Obesity: more stress, due to weight, on your spine can accelerate spinal degeneration.
- Sedentary lifestyle: Sitting for long periods of time can contribute to the development of sciatica.
- Muscular weakness: Our spines need to be properly supported by the surrounding muscles. When these muscles are weak, the underlying spine is at risk.
- Diabetes can lead to an increased risk of nerve damage.
Diagnosis
Sciatica is diagnosed based on the examination findings by your physician or physiotherapist. Imaging isn’t required in most cases. If the patient has a past medical history of disabling symptoms, osteoporosis, steroid use, unexplained fever/weight loss, tumour history, trauma and/or IV drug use imaging may be necessary.
If a patient does not have an improvement in symptoms from rest, physical therapy and medication after 3 months then an MRI may be recommended to evaluate their candidacy for surgery.
How Long Does Sciatica Last?
Most cases of sciatica resolve within 3-5 months. Some more severe cases will take a year. Physiotherapy should be the treatment of choice to deal with sciatica. In fact, surgery does not improve a patient's outcome from sciatica, but it may shorten the amount of time for the condition to resolve for a small percentage of patients.
Principles of Physiotherapy for Lumbar Disc Herniation Causing Sciatica
Every case of sciatica is as different as the individual it is effecting. This is why it is important to be assessed by an experienced physiotherapist. The treatment plan should address the major factors leading to the development of sciatica for that patient. Here are a few common problems that may be contributing to your sciatica and how to address them.
- Poor sitting/driving posture - Make changes to your workstation or car seat to ensure these activities are not making you worse.
- Poor lifting technique - Your Physiotherapist can teach you how to lift objects while properly supporting and protecting your spine.
- Poor core strength - an exercise program to improve your strength may be required.
- Poor spinal mobility - a stiff spine is at risk of developing pain. You may need to include mobility exercises.
- In the acute stages, your therapist may use pain-relieving manual therapy or modalities like acupuncture to help provide relief.
If non-operative treatment fails and patients continue to experience radicular (leg dominant) symptoms, a nerve root injection and/or surgical intervention may be considered.
Final Thoughts on Sciatica
Left untreated most people who develop sciatica will have frequent recurrences of pain that last weeks to months. But patients who undergo a well-designed physiotherapy program and participate in prevention can dramatically reduce the number and intensity of recurrences. If you are struggling with sciatica, get in to see your physiotherapist right away.
Our Pricing
Our Pricing
Our services are reimburseable through most private insurance providers including Cowan, Great-West Life, Desjardins, iA Financial Group, and Standard Life.
Physiotherapy
/45 min session
Licensed Physiotherapist
Personalized treatment plan
Direct billing available
Virtual Physiotherapy
/60 min session
Licensed Physiotherapist
Personalized treatment plan
Direct billing available
Massage Therapy
/60 min session
Registered Massage Therapist
Enhances physical well-being
Direct billing available
Psychotherapy
/60 min session
Licensed Psychotherapist
Promotes long-term wellness
Direct billing available

